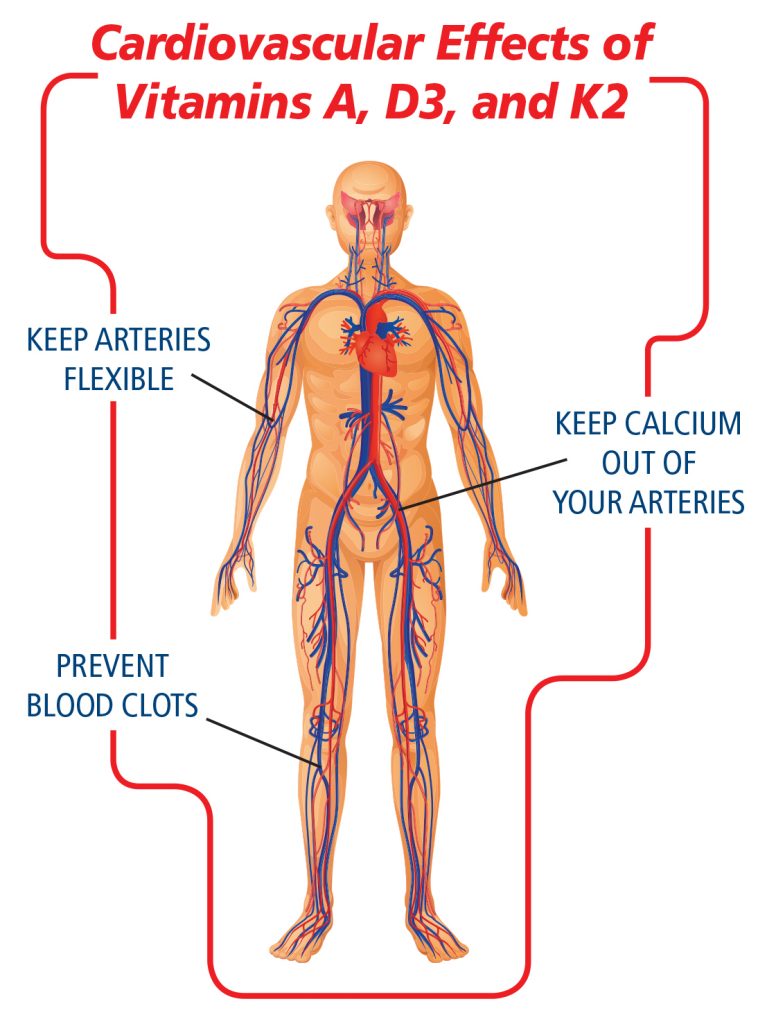
PREVENT HEART DISEASE WITH VITAMINS A, D3, AND K2
If you have patients with high blood pressure, stroke, clogged arteries, or other cardio concerns, there are three nutrients they should consider. These ingredients strengthen blood vessels, increase their natural flexibility, and keep calcium where it belongs. They reduce the risk of heart disease without the side effects of calcium channel blockers or other drugs.
INFOMEDICA’S BOTTOM LINE:
Vitamins A, D3, and K2 are the unsung heroes of our cardiovascular system. This trio of fat-soluble vitamins team up to ensure the proper function of the heart and the 60,000 miles of blood vessels. Yet most people don’t know how important it is to get enough of all three. And that lack of knowledge just might be slowly killing them.
Vitamins A, D3, and K2 work as partners to:
- Keep calcium in your bones and out of the arteries
- Prevent dangerous blood clots, heart attacks, and high blood pressure
- Help keep arteries flexible and strong
- Reduce inflammatory markers in the bloodstream
Calcium plays a key role in cell signaling, blood clotting, and muscle contractions—including that most important muscle, the heart. But calcium also has a dark side.
The Calcium Paradox: Good, Bad, or Both?
If calcium is not properly regulated in the blood and tissues, calcium can build up in the body as we age—a process called calcification. Some calcification is relatively harmless. For example, half of all women over fifty will show some benign calcification in breast tissue during a mammogram. However, this accumulation may be an indication of further calcium build up in other areas of the body, like the arteries and the heart. This makes arteries stiff and inflexible, leading to increased risk of blood clots, strokes, and heart attacks. This negative aspect of calcium is sometimes called the Calcium Paradox—too little calcium in bones and too much in the arteries.
If your patients have been taking a calcium supplement, and wonder if it could be having a negative effect on their heart, they may be tempted to stop supplementing. But their bones need the mineral to stay strong, too.
You can assure them that what they really need is to make sure they are getting enough of the nutrients that regulate calcium: the fat-soluble vitamins K2, D3, and A.
Vitamin K2: A Key Nutrient for Blood Coagulation
Vitamin K comes in two forms: vitamin K1 (phylloquinone) and vitamin K2 (menaquinone). Vitamin K1 is the form associated with coagulation to prevent excessive bleeding in cases of wounds and injuries. The body uses vitamin K2 to activate proteins, such as osteocalcin and matrix GLA-protein (MGP), that help carry calcium to where it’s needed. Osteocalcin puts calcium into bone tissue, making the bones stronger. MGP inhibits calcium accumulation in the arteries and other body tissues. Optimal levels of vitamin K2 ensure these proteins work the way they should.
The lower the intake of vitamin K2, the greater the risk of heart disease and a heart attack. The Rotterdam study, a large population-based study of older Dutch adults, looked at the relationship between vitamin K2 and coronary heart disease (CHD). Those who had a higher dietary intake of vitamin K2 had a lower risk of death from CHD and severe aortic calcification. A 2012 study published in the Journal of Bone and Mineral Research examined patients with kidney disease. These patients develop calcium deposits in their arteries at twice the rate of the general population. In this study, more than a third of the patients were deficient in vitamin K, and those patients with low levels of vitamin K2 had significantly higher levels of calcification.
Vitamin D3: The sunshine vitamin is crucial to bone and heart health, but few people get enough of it. That’s unfortunate, because it’s a required nutrient for calcium absorption and metabolism, as well as for bone formation and bone density. Vitamin D is also used by many cells in the cardiovascular system, including heart muscle cells and the cells that line the blood vessels. Low levels of vitamin D in the blood have been linked to a greater risk of dying from heart disease or stroke. Additionally, vitamin D has been found to decrease inflammatory markers associated with heart disease, such as C-reactive protein.Vitamin D helps prevent calcium buildup in the blood vessels. It increases the expression of those vitamin K-dependent proteins that regulate calcium. Without enough of those proteins, calcium can’t get to bones and instead accumulates in the blood vessels and artery walls, causing stiffening. Of course, optimal levels of vitamin D require enough vitamin K to activate those proteins. Studies are finding that vitamin D and vitamin K work better when they’re both at optimal levels.
Vitamin A: Science is still piecing together the multiple effects of vitamin A in the body. While vitamin A is widely known for being essential for healthy eyes, it does so much more. It influences a number of body processes, including regulating various proteins that control the types of cells the body makes. This includes the cells that line blood vessels. In addition, vitamin A levels drop rapidly when inflammation is present, signaling its vital role in fighting disease and injury.
The form of vitamin A used in the body is retinol. Many multivitamins have replaced their retinol forms of vitamin A with beta-carotene. But beta-carotene isn’t the same as vitamin A, it’s a provitamin A carotenoid. It must be changed into retinol in the body in order for it to be useful. In addition, the absorption of beta-carotene can be low and is dependent on many factors, including genetic variations and whether it was consumed with fat (which improves absorption).
Researchers investigating the relationship between vitamins A, D3 and K2, have discovered that Vitamin A and D appear to work together. They are involved in the communication between cells, especially those cells involved in calcium regulation via vitamin K-dependent proteins.
A Healthy Heart Requires A Delicate Balance
Researchers are still finding out a lot about the requirements of a healthy heart and arteries. But one thing that keeps emerging is really just common sense—nutrients don’t work in isolation. The combination of vitamins A, D3, and K2 helps put calcium where it’s needed, and keeps it from settling where it isn’t. In addition, these vitamins have a direct impact on the way the heart and arteries respond to daily challenges.


